Can An Osteopath Help With Sciatica?
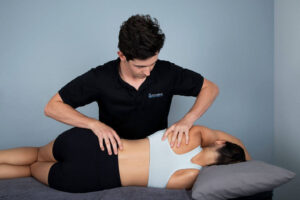
Sciatica is a common and often debilitating condition that affects millions of people, causing pain, tingling, or numbness that travels from the lower back down through the legs. For many sufferers, the journey to relief is filled with questions—especially when exploring treatment options beyond medication or surgery. As Osteopath’s we see this presentation daily. As common as this problem is, sadly it is also filled with myths’ false claims and misinformation.
For people who have never experienced an Osteopathy treatment session, you’re likely wondering: Can osteopathy really help with nerve pain? What does an osteopath actually do during treatment? How many sessions will I need? Is it safe or suitable for my specific case?
This blog explores these common questions and demystifies what osteopathic treatment for sciatica involves. We’ll look at how osteopaths assess and treat the root causes of sciatic pain, what you can expect during your first session, and what you can do to help yourself outside of our sessions! Whether your sciatica is recent or something you’ve been managing for years, understanding your options can help you make an informed choice about your recovery.
 What Can Cause Sciatica and how does Osteopathy address these Causes?
What Can Cause Sciatica and how does Osteopathy address these Causes?
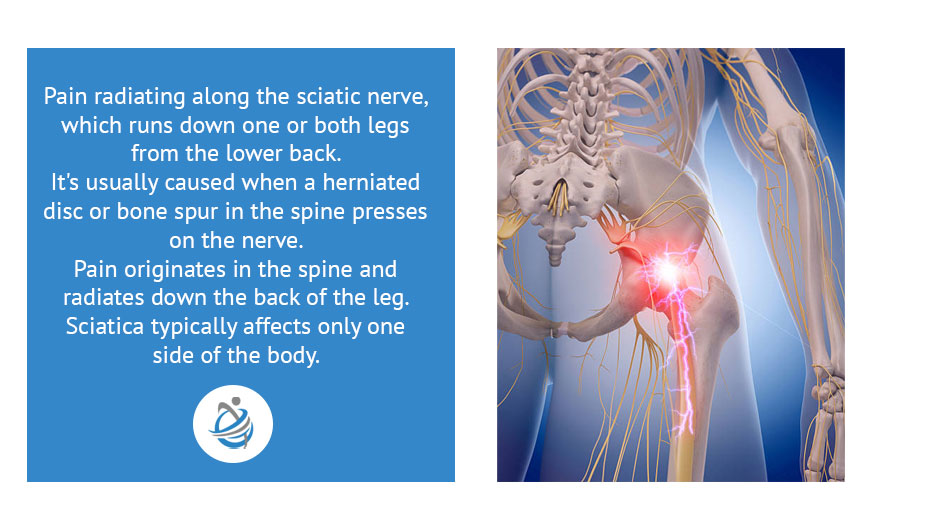
Sciatica is most commonly caused by compression or irritation of the sciatic nerve. There are a number of different structures in our body that can cause this pain. The more common causes are often due to a herniated or degenerated disc, or nerve root compression in the lumbar spine. As Osteopaths aim to address the root cause of the pain. We aim to improve spinal and hip mechanics, relieve muscle tension and joint restriction. By improving biomechanics and relieving muscle spasm and tension the body can move properly again. And in conjunction with a strengthening and mobility program you can start to live your life without the pain of Sciatica.
Can An Osteopath Really Help With Sciatica? And How Effective Is It?
This is a very common question our Glen Iris Osteopath’s often get asked. The simple and quick answer is Yes, osteopathic treatment can be effective for sciatica!. Osteopaths use gentle manual techniques to relieve pain, reduce muscle spasm, and improve mobility. Whether the pain is acute or chronic we are well equiped to help you overcome your pain and irritation. And get you back to doing the thins you love to do, Pain free! Treatments are tailored to the individual, and every patient will also get a unique management plan and pathway forward.
What Are The Common Symptoms Of Sciatica?
Sciatica refers to pain caused by irritation or compression of the sciatic nerve, which runs from the lower back down through the hips, buttocks, and legs. Symptoms can vary in intensity and location, but commonly include:
Lower back pain that may radiate through the hip and down the leg
Pain in the buttock, thigh, leg, or foot, often described as sharp, burning, or shooting
Numbness or tingling, often in the back of the leg or foot
Muscle weakness in the leg or foot
Pain that worsens with prolonged sitting, standing, or certain movements like bending or twisting
These symptoms typically affect one side of the body, though in rare cases both legs may be involved.
Conservative treatment like osteopathy is usually the first-line treatment for relieving, treating, and preventing sciatica symptoms. Typical sciatica signs and symptoms through physical therapy include:
What Does An Osteopath Do During A Sciatica Treatment Session?

Our Goals of treatment are:
- Restore pain-free functional movement patterns
- Relieve lower back pain, buttock, thigh, and leg pain
- Reduce muscle spasm
- Restore function of the lumbar spine and the sacroiliac joints
- Improve mobility of the lower body
- Foster a better healing environment in the lower back
- Prevent future pain flareups and reduce fear associated with movement
- Provide home based strengthening program to build resilience and tolerance.
What type of techniques due Our Osteopath’s Use?
To begin with, each and every patient is different. As is tolerance to certain techniques. We use a wide variety of techniques which suit you specifically and give you the best results
Common techniques used by an osteopath to treat sciatic:
- Strengthening exercises include bodyweight and resistance exercises to strengthen the muscles of the abdomen, low back, hips, and legs.
- Functional retraining includes reintroducing movements, such as lifting, carrying, and bending or squatting. The use of proper technique and healthy movement patterns are incorporated to reduce pain and prevent re-injury.
- Nerve glides (nerve mobilization) involves active or passive techniques on a symptomatic nerve when it is placed into and out of tension to facilitate movement and reduce symptoms.
- Joint mobilization is a manual therapy technique in which the therapist applies pressure to a joint to mobilize it and produce a therapeutic effect.
- Joint manipulation is a gentle manual technique in which the therapist applies a quick short thrust of motion of a joint to promote improve movement
- Dry needling is a technique in which a small needle is inserted into the tight muscles to help release hyper-irritable and/or hyper-contracted muscle tissue to reduce pain.
- Muscle energy technique is a form of manual therapy that involves the patient performing gentle muscle contractions in conjunction with the therapist moving your joints through a specific range of motion. This technique may help reduce pain and restore function.
- Soft tissue Massage – a great technique to help decrease muscle tension or spasm.
- Gait training includes analysis of walking technique and retraining correct gait patterns. This technique may include video analysis.
- Active assisted range of motion includes therapist-assisted movement of parts of the lower body, such as the hip and legs. This technique helps facilitate the movement of specific joints or muscles that cause pain.
Every patient will have a different presentation, which means some or all of these different treatment techniques may be used in your session.
In addition to physical therapy and exercise, committing to correct and ergonomically supported posture while sitting, standing, and walking is essential in treating and preventing sciatica. Daily routines, such as following ergonomically safe lifting techniques and using good sleep postures are also important to follow.
What Exercises can Help with sciatic Symptoms?
Please keep in mind these are very general exercises. They may not be suitable for everyone. We highly recommend getting an assessment from a qualified practitioner to ensure these exercises are not going to flare up your condition. The first question you should ask yourself is, do you actually “have” Sciatica! Many problems can mimic sciatica.
Here are our 3 Favourite exercises to help sciatica!
1: Mckenzie Back Extension
2: Dead Bug:
3: Dead Lift
Final Thoughts on Glen Iris Osteopathy for Sciatica
When sciatica flares up, the pain can be intense and sometimes overwhelming. While a short period of rest—one or two days—may help ease acute discomfort, extended inactivity is generally discouraged. Prolonged rest can actually worsen symptoms by increasing stiffness, and contributing to muscle de conditioning. Gentle movement is essential to promote healing and restore function.
Osteopathic care can play a vital role in both relieving symptoms and preventing future episodes. Osteopathy, in particular, focuses on improving the body’s natural mechanics, addressing the underlying causes of nerve irritation, and supporting long-term recovery through tailored hands-on treatment.
If you’re living with sciatica, there are effective, non-invasive options available. At Equilibrium Sports and Spinal Clinic in Glen Iris, we pride ourselves on delivering the highest quality care delivering comprehensive treatment sessions tailored to your needs.
Don’t let sciatica control your life—book your appointment today and start your journey toward lasting relief.


 What Can Cause Sciatica and how does Osteopathy address these Causes?
What Can Cause Sciatica and how does Osteopathy address these Causes?