Please, before reading this article, check out our first blog post on pain.
Examples of pain to get you thinking;
I think there examples of people in pain that can make us question the origins/influences of pain.
- Phantom Limb Pain – Phantom limb pain is pain someone experiences after a limb amputation. They can feel pain in their big toe that isn’t there anymore.
- Paper cut – the most painful thing for two minutes. After that, you can look at the cut, which hasn’t now healed, and you’d be able to flick it and it won’t hurt.
- Sporting injuries – There are times during the game where players will get cuts, bruises, etc., and not realise until they finish. This is because in the context of the game, there are more important things to focus on.
- Plucking a hair – Plucking a single hair can cause quite a sharp pain. Even when we know it is not causing any significant damage.
These few examples hopefully get you thinking about how pain and how complex it can be. More often than not our perception of pain in these situations (and many more situations) are not directly related to how much damage there is.
It has been shown that the same areas in the brain that get activated when someone is receiving nociceptive inputs from their nervous system, also get activated in other situations. These areas in the brain are called the “pain matrix” collectively. The pain matrix can be activated when a threat is seen in the persons environment without causing any nociception. For example, a wasp flying close to the body can activate the pain matrix, even though their has been no insult on the body. This shows the complexity of our brain and how pain can be affected by many things.
What influences pain?
We’ve (pain scientists, and in turn health practitioners) learned that pain doesn’t always match up with how damaged our tissues are. If you’ve had pain for a while, you’ve probably noticed that some days are worse, some are better, and it can even change from day to day. But why does this happen? Is it because your body is healing one day and getting worse the next? Well, it’s actually more complex than that. Pain doesn’t always have a direct link to how your body is healing.
So what influences those fluctuations of pain? I think the low hanging fruit are the common health metrics we all hear about from government initiatives, including;
factors outside of damage affecting pain:
- Diet – be it “healthy” or “unhealthy”
- water consumption
- amount of sleep
- how much exercise someone does
- alcohol consumption
- smoking status
But there are other factors that can affect someones level of pain day to day or week to week. For example:
- family stress
- work stress
- mental health status
- emotional stress
- previous pain experiences
- beliefs around pain
- family history of pain
I frequently discuss these factors with clients, not so they go home, flip their life around and change everything, but to give themselves a break when they’re in pain. Their increase in pain likely isn’t due to more damage, so they can cut themselves some slack. All of these factors can contribute to our nervous system having a lower threshold to pain, meaning that smaller things can flare you up.
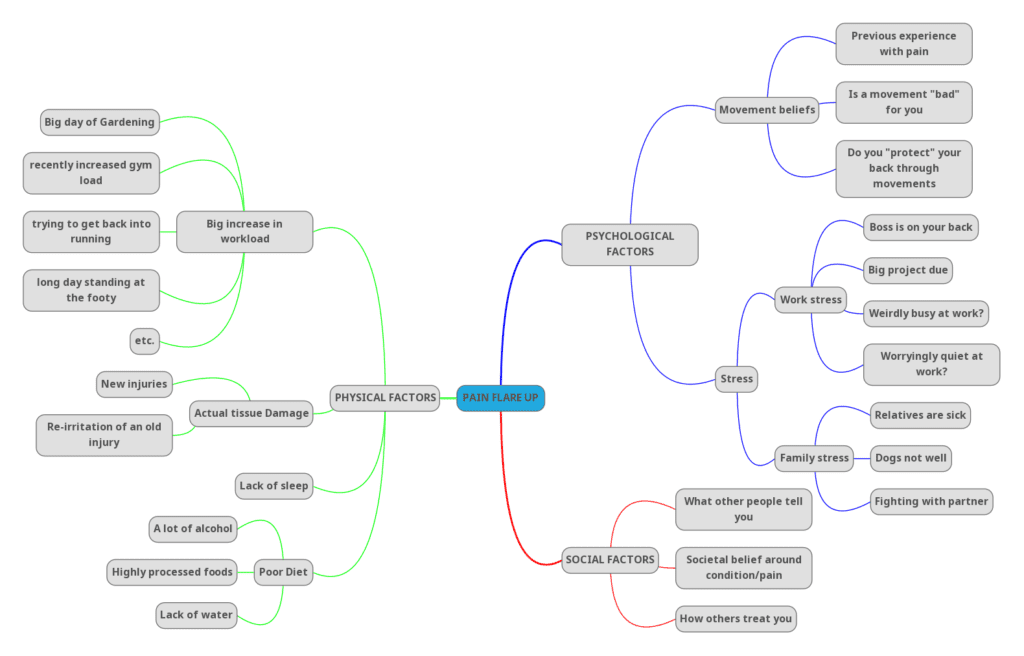
So What Can You Do in a Flare-up?
My first piece of advice would be to see a health professional to confirm that the flare-up of pain isn’t more damage/anything sinister. Once that has been ticked off there are plenty of things you can do. Here is a list I like to do if my hip (injured 4 years ago in cricket) has a flare-up, but can be applied to any body part:
- Instead of googling, use your practitioner of choice as your google. Get reassurance from them, not WebMd
- Remind myself that more damage is unlikely because the human body is strong and adaptable
- test what movements I can do. Which ones make me feel worse (sensitisation), which ones make me feel better (habituation)
- If I am in quite a bit of pain, do the movements that make me feel better and repeat them to build confidence
- If I’m feeling up to it, sometimes testing the painful movements can help desensitise ourselves to those movements
- I would do the painful movement until I feel a 3 or 4 out of 10 pain limit and then return to starting position
- Seek advice about pain medications if the pain is unbearable (pharmacist, GP etc.)
-
What can we control when we’re in pain? take control of things I can control:
- diet
- water intake
- sleep
- wellness activities, things that you enjoy doing
- yoga
- sauna
- ice bath
- breath work
- walking the dogs
- stretching
- gardening
- cooking
- etc. (these are different for everyone)
Summary
- Pain is a very complex, individual experience that has many, many factors playing into it.
- THERE IS A DIFFERENCE BETWEEN PAIN AND DAMAGE
- Because of the complexity of pain, when we are in it, there is an abundance of different options we can trial to help ourselves
- movement is often a great way to decrease sensitivity in a painful area
- Be brave when in pain, test what hurts and build a plan of how to desensitise the painful area
- Humans are robust, adaptable organisms that heal and change. We can improve our pain experience, so don’t lose hope
Further Readings/information
There are some fantastic resources out there that can help people in pain. Here are two to get you started.
- Tame the beast – A great website by leading pain scientists in Australia. Watch their video
- Pain Australia – navigate your way to the “About Pain” tab
** Our osteo, Kieren Jamieson, is currently studying a Master’s of Science in Medicine (Pain Management)**
Please reach out to us if you have any questions. You can reach us via email (info@equilibriumsas.com.au), instagram and by phone (03 9822 1900). We will get back to you as soon as we can.
If you need an appointment, please follow this link and book in. BOOK HERE